What are the symptoms of Malaria?
Overview I Pathogenesis I what are the symptoms of malaria? I Causes I Diagnosis I Complication I Long term outlook of malaria I Preventions
Overview
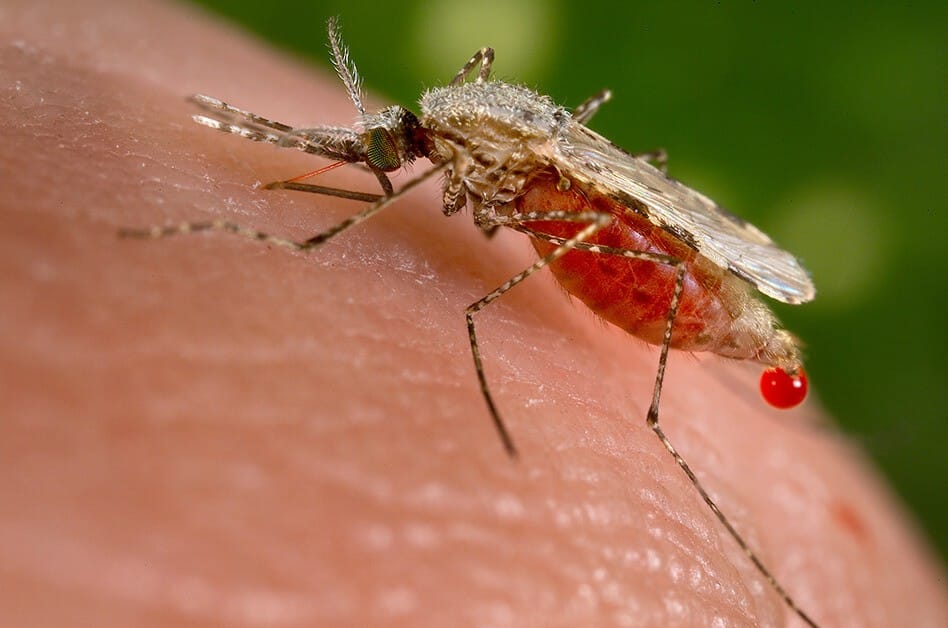
Malaria is a life-threatening disease. It is transmitted through the bite of the infected Anopheles mosquitoes. When the mosquitoes bite you, the parasite is released into the bloodstream. Malaria is also a mosquito-borne infectious disease. It affects humans and other animals that is caused by parasitic single-celled microorganisms belonging to the Plasmodium group. In a severe case, it causes yellow skin, seizure, coma and death. Symptoms usually begin ten to fifteen day after being bitten by an infected mosquito. Do you know what are the symptoms of Malaria? Malaria causes symptoms that typically include fever, tiredness, vomiting, headaches and other systematic symptoms.
The risk of disease can be reduced by preventing bites through the use of mosquito net and insect repellents. it can also reduce with mosquito control measures such as spraying insecticides and draining standing water. Several medications are available to prevent malaria in travellers to the area in which disease is common. Occasional doses of the combination medications (anti-malarials medications) sulfadoxine/pyrimethamine are recommended in infants and after the first trimester of pregnancy in areas with high incidences of malaria or the high risk of malaria. Despite a need, no effective vaccine exists, although the effort to develop is going on.
The disease is widespread in tropical and subtropical regions that exit in broadband around the equator. Malaria includes much of sub-Saharan Africa, Asia and Latin America travellers are susceptible to malaria. most cases are due to P. falciparum, usually, from Africa, and of these 1% cases, the patient dies because of late diagnosis.
Migrants from endemic countries who spend long periods of time in non-endemic countries are particularly at risk if they visit friends and family in their country of origin. They have lost their partial immunity and frequently do not take malaria prophylaxis. A few people living near airports in Europe have acquired malaria from accidentally imported mosquitoes.
Pathogenesis
The life cycle of the malaria parasite
The female anopheline mosquito becomes infected when it depends on human blood containing gametocytes, the sexual forms of the malaria parasite. Development in the mosquito takes 7-20 days and results in sporozoites accumulating in salivary glands. And being inoculated into the human bloodstream.
Sporozoites disappear from human blood within half an hour of infection and enter into the liver. After some days. Merozoites leave the liver and permeate red blood cells, where further asexual cycles of multiplication take place, producing schizonts. Rupture of the schizont releases more merozoites into the blood and causes fever, the periodicity of which depends on the species of parasite.
P.vivax and P.ovale may live in liver cells as dormant forms, hypnotizes, capable of developing into merozoites months or year later. Thus the first condemn of clinical malaria may occur long after the patient has left the endemic area, and the disease may get worse again after treatment with drugs that only kill the erythrocytic stage of the parasite.
P.faliparum, p.knowlesi and P.malariae have no tenacious exo-erythrocytic phase but recrudescence of fever may result from the multiplication of parasites in red cells that have not been eliminated by treatment and immune processes.
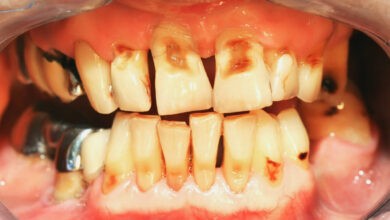
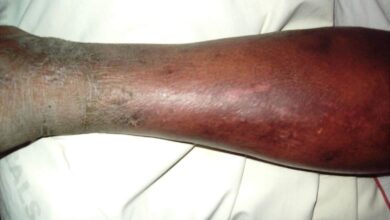
What are the Symptoms of malaria?
The symptoms of malaria typically start to develop within 10 days to 4 weeks following the infections. In some case, symptoms may not develop for several months. some malarial parasite can enter the body but will not dormant for the long periods of time.
- High fever with chill and rigors (evening rise of temperature)
- stage of fever
- High Temperature
- Shivering and cool
- -sweating
- Headache
- Nausea
- Vomiting
- Anaemia
- Abdominal pain
- Muscle pain
- Convulsion
- • Coma
- • Bloody stool
Systematic clinical features are:
Neurological
- Coma hypoglycaemia
- Seizures
- Cranial nerve palsies
- Opisthotonus
- Optic fundi
Respiratory
- Pulmonary oedema
- Secondary bacterial pneumonia
Cardiovascular
- Shock
- Cardiac failure
- Dysrhythmias with quinine
Renal
- Acute kidney injury
- Severe haemolysis resulting in haemoglobinuria (‘blackwater fever’)
Abdomen
- Jaundice
- Tender liver edge with hepatitis
- Pain in the left upper quadrant with splenomegaly
Blood
- Parasitemia
- Anaemia
- Thrombocytopenia
- coagulopathy
What causes Malaria?
Malaria can occur if mosquito infected to Plasmodium parasites bites you. There is four kinds of malarial parasite that can affect humans.
a) Plasmodium Vivax
b) Plasmodium Ovale
c) Plasmodium Malariae
d) Plasmodium Falciparum
P. falciparum causes more severe and more complications than other disease and those who contract this form of malaria have a high risk of death. A newborn baby also gets infected from his/her infected mother at the time of birth. This is known as congenital malaria.
Malaria is transmitted through the blood and also it can be transmitted through
- an organ transplant
- a transfusion
- use of shared needles or syringes
How is MALARIA diagnosed?
When you visit your doctor, your doctor will be able to diagnose malaria. Your doctor will review your health history including travel histories like travelling to an endemic area or any recent travel to tropical climates.
The doctor will be able to determine if you have enlarged spleen or liver. If you have symptoms of malaria, your doctor may advise an additional blood test to confirm the diagnosis.
These test will show:
- Whether you have malaria
- What type of malaria you have
- if your infections are caused by a parasite that is resistant to certain types of drugs
- In the case that disease caused anaemia
- if a disease has affected your vital organ
Life-Threatening Complications of Malaria
- malaria can cause a number of life-threatening complications. Some of them are:
- Swelling of the blood vessel of the brain, or cerebral malaria
- pulmonary oedema (an accumulation of fluid in the lungs that causes breathing problems
- organ failure of kidney, liver, and spleen
- anaemia occurs due to Red blood cell(RBC) destruction
- low blood sugar
Schematic illustrations of life cycle P.falciparum
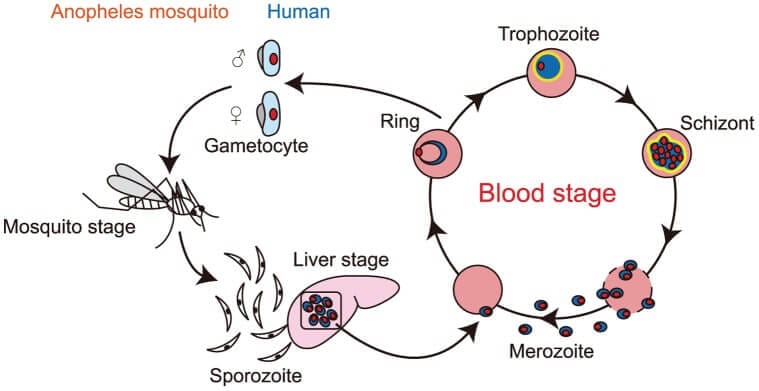
How is malaria treated?
Malaria can be life-threatening if you have infected with parasite Plasmodium falciparum. The treatment of disease is typically provided in the hospital. In some instance, the medications prescribed may not clear the infections because of parasite resistance to drugs. If this occurs, your doctor may need to use more than one medications or change medications altogether to treat your conditions.
Additionally, a definite type of malaria parasites such as P.Vivax, P.Ovale has liver stages where these parasites can stay in your body for an extended period of time and also revive at later date causing a relapse of infections.
If you’re found to have one of these types of malaria parasites, you will be given a second medication to prevent relapse in future.
What’s the long term outlook for people with malaria?
People with malaria who receive treatment typically have a good long-term outlook. If complications arise a result of malaria, the outlook may not be good. cerebral malaria which causes swelling of blood vessels of the brain results in brain damage.
The long-term-outlook off patients with drugs resistant parasite may be also poor. In these patients, malaria may recur. These may cause other complications.
Preventions
Clinical attacks of malaria may be preventable with chemoprophylaxis using chloroquine, atovaquone plus proguanil (Malarone), doxycycline or mefloquine, give the recommended doses for protection of the non-immune. The risk of malaria in the area to be visited and the degree of the chloroquine resistance guide recommendation prophylaxis. And here are some other health tips to prevent malaria
- Determine your level of risks.
- Stay in the well -screened area at night.
- Always use a bed.
- Use mosquito repellent.
- •Go for long sleeves
- Insect repellent again
- Sunscreen comes the first-repellent second.
- check malaria risk-get the anti-malaria(if necessary)
- Follow your prescriptions carefully
- Be on safe sides