Non-alcoholic fatty liver disease

Increasingly sedentary lifestyles and changing dietary patterns mean that the prevalence of obesity and insulin resistance has increased worldwide, and so far accumulation in the liver is a common finding during abdominal imaging studies and on liver biopsy. In the absence of high alcohol consumption (typically, a threshold of <20 gm/day for women and 30 gm/day for men is adopted), this is called non-alcoholic fatty liver disease (NAFLD).
Non-alcoholic fatty liver disease(NAFLD) includes a spectrum of progressive liver disease ranging from fatty infiltration alone (steatosis) to fatty infiltration with inflammation (non-alcoholic steatohepatitis, NASH) and may progress to cirrhosis and primary liver cancer. Non-alcoholic fatty liver disease(NAFLD) is considered by many to be the hepatic manifestation of the ‘metabolic syndrome’, as it is strongly associated with obesity, dyslipidaemia, type 2 diabetes and hypertension. Estimated vary between populations, although on large European study found NAFLD to be present in 94% of obese patients (body mass index 9BMI)>30 kg/m²), 67% of overweight patients (BMI>25kg/m²) and 25% of normal-weight patients. The overall prevalence of Non-alcoholic fatty liver disease (NAFLD) in patients with type 2 diabetes ranges from 40% to 70%. Histological non-alcoholic steatohepatitis has been found in 3-16% of apparently healthy potential living liver donors in Europe and 6-15% in the USA.
Overall, NAFLD is estimated to affect 20-30% of the general population in western countries and 5-18% in Asia, with about 1 in 10 NAFLD cases exhibiting NASH. The frequency of steatosis varies with ethnicity (45% in Hispanics, 33% in whites and 24% in blacks) and gender (42% white male versus 24% white females) but only a minority of patients will progress to cirrhosis and end-stage liver disease. However, because obesity is common and the prevalence of NAFLD is rising, this still represents a large number of patients, placing a substantial burden on health-care resources.
Over a median 12-year follow-up period in a cohort of 619 NAFLD patients, an overall 33.2% risk of death or liver transplantation was observed, with liver-related mortality being the third most common cause of death after cardiovascular disease and extrahepatic malignancy. Non-alcoholic fatty liver disease is the leading case of liver dysfunction in the non-alcoholic, viral hepatitis-negative population in Europe and North America, and is predicted to become the main aetiology in patients undergoing liver transplantation during the next 5 years.
Pathophysiology
The initiating event in Non-alcoholic fatty liver disease is based on the development of obesity and insulin resistance, leading to increased hepatic free fatty acid flux. This inequality between the rate of import/synthesis and the rate of export/catabolism of fatty acids in the liver leads to the development of steatosis. This may be an adaptive response through which response through which hepatocytes store potentially toxic lipids are relatively inert triglyceride. A ‘two-hit’ hypothesis has been proposed to describe the pathogenesis of NAFLD, the ‘first hit’ causing steatosis that then progresses to non-alcoholic steatohepatitis if a ‘second hit’ occurs. In reality, progression probably follows hepatocellular injury caused by a combination of several different ‘hits’, including:
- Oxidative stress due to free radicals produces during fatty acid oxidation
- Direct lipotoxicity from fatty acids and other metabolites in the liver
- Endoplasmic reticulum stress
- Gut-derived endotoxin
- Cytokine release (TNF-ɑ etc.) and immune-mediated hepatocellular injury.
Cellular damage triggers cell death and inflammation, which leads to stellate cell activation and development of hepatic fibrosis that culminates in cirrhosis. As with much other liver diseases, subtle inter-patient genetic variations and environmental factors interact to determine disease progression. Several genetics modifiers of disease severity have been identified, with PNPLA3 and its product, adioponutrin, being the best validated.
This should not be confused with acute fatty liver, which can occur in hepatic mitochondrial cytopathies, e.g. acute fatty liver of pregnancy, or in other situations, e.g. Reye’s syndrome or drug toxicity (sodium valproate, tetracyclines), or with bacterial toxins (e.g. Bacillus cereus). In these, defective mitochondrial beta-oxidation of lipids leads to fat droplet accumulation in hepatocytes and microvesicular steatosis.
Clinical features
Non-alcoholic fatty liver disease is frequently asymptomatic, although it may be associated with fatigue and mild upper quadrant discomfort. It is commonly identified as an incidental biochemical abnormality during routine blood tests or as fatty liver during an ultrasound or CT scan of the abdomen. Alternatively, patients with progressive non-alcoholic steatohepatitis may presents late in the natural history of the disease with complications of cirrhosis and portal hypertension, such as variceal haemorrhage, or with hepatocellular carcinoma.
The average age of NASH patients is 40-50 years (50-60 years for NASH-cirrhosis); however, the emerging epidemic of childhood obesity means that NASH is present in increasing numbers of younger patients. Recognised independent risk factors for disease progression are age over 45 years, presence of diabetes (or severity of insulin resistance), obesity (BMI >30kg/m²) and hypertension. These factors help with identification of ‘high-risk’ patients groups. NAFLD is also associated with polycystic ovary syndrome, obstructive sleep apnoea and small-bowel bacterial overgrowth.
Risk factor
A wide range of disease and conditions can increase your risk of non-alcoholic fatty liver disease, including
- High cholesterol
- High levels of triglyceride in the blood
- Metabolic syndrome
- Obesity, particularly when fat is concentrated in the abdomen
- Polycystic ovary syndrome
- Sleep apnea
- Types 2 diabetes
- An underactive thyroid (hypothyroidism)
- Underactive pituitary gland (Hypopituitrasim)
Non-alcoholic steatohepatitis is more conjecturable in these groups:
- Older people
- People with diabetes
- People with a high amount of body fat concentrated in the abdomen
It is difficult to distinguish the non-alcoholic fatty liver disease from non-alcoholic steatohepatitis without further testing.
Investigations
Investigations of patients with suspected non-alcoholic fatty liver disease should be directed first towards the exclusion of excess alcohol consumption and other liver diseases (including viral, autoimmune and other metabolic causes) and then at confirming the presence of NAFLD, discriminating simple steatosis from non-alcoholic steatohepatitis and determining the extent of any hepatic fibrosis that is present.
Biochemical tests
There is no single diagnostic test for NAFLD. Elevations of serum ALT and AST are modest and usually less than twice the upper limit of normal. ALT levels fall as hepatic fibrosis increases and the characteristics AST: ALT ratio of <1 seen in NASHreverses (AST: ALT>1) as diseased progress towards cirrhosis, meaning that steatohepatitis with advanced disease may be present even in those with normal-range ALT levels. Other laboratory abnormalities that may be present include non-specific elevations of GGT, low-titre antinuclear antibody (ANA) in 20-30% of patients and elevated ferritin levels.
Although routine blood tests are unable to determine the degree of liver fibrosis/cirrhosis accurately, calculated scores, such as the NAFLD fibrosis score and FIB-4 score, which are based on the results of routinely available blood tests and anthropometrics, have a high negative predictive value for advanced fibrosis/cirrhosis and so can be used to rule out advanced fibrosis in many NAFLD patients. This allows care to focus on those most likely to have advanced disease.
Imaging
Ultrasound is most often used and provides qualitative assessments of hepatics fat content, as the liver appears ‘bright’ due to the increased echogenicity, sensitivity is limited when fewer than 33% of hepatocytes are steatotic, however, CT, MRI or MR spectroscopy often greater sensitivity for detecting lesser degrees os steatosis, but these are resources- intensive and not widely used. NO routine imagining modality can distinguish simple steatosis from steatohepatitis or accurately quantify hepatic fibrosis short of cirrhosis.
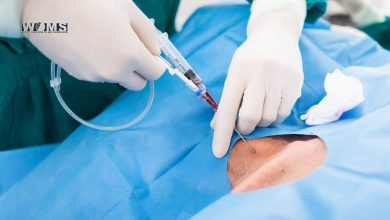
Liver Biopsy
Liver biopsy remains the ‘gold standard’ investigation for diagnosis and assessment of a degree of inflammation and extent of liver fibrosis. The histological definition of non-alcoholic steatohepatitis is based on a combination of three lesions (Steatosis, hepatocellular injury and inflammation; with mainly centrilobular, acinar zone 3 distribution. Specific features include hepatocytes ballooning degeneration with or without acidophil bodies or spotty necrosis and a mild, mixed inflammatory infiltrate. These may be accompanied by Mallory-Denk bodies (also known as Mallory’s hyaline). Perisinusoidal fibrosis is a characteristics features of NASH. Histological scoring systems are widely used to access disease severity semi-quantitatively.
It is important to note that hepatic fat content tends to diminish as cirrhosis develops and so NASH is likely to be under-diagnosed in the setting of advanced liver disease, where it is thought to be the underlying cause of 30-75% of cases in which no specific aetiology is readily identified (so-called ‘cryptogenic cirrhosis’).
Management
As it is a marker of the metabolic syndrome, identification of NAFLD should prompt screening for and treatment of cardiovascular risk factors in all patients. It is also necessary to access whether patients. It is is also necessary to access whether patients have progressive disease and advanced fibrosis so that liver-targeted treatment can be focused particularly on those patients. While the liver biopsy is best able to do this, it is invasive and unsuitable for widespread use outside the specialist care setting. An example of an algorithm for the assessment and risk stratification of patients with NAFLD.
Non-pharmacological treatment
Current treatment comprises lifestyle interventions to promote weight loss and improve insulin sensitivity through dietary changes and physical exercise. Sustained weight reduction of 7-10% is associated with significant improvement in histological and biochemical non-alcoholic steatohepatitis severity.
Pharmacological treatment
No pharmacological agents are currently licensed specially for NASH therapy. Treatment directed at coexisting metabolic disorders, such as dyslipidaemia and hypertension, should be given. Although the use of HMG-CoA reductase inhibitors (statins) does not ameliorate NAFLD, there are does not appear to be an increased risk of hepatotoxicity or other side-effects from these agents, and so they may be used to treat dyslipidaemia. Specific insulin-sensitising agents, in particular, glitazones, may help selected patients, while recent results with bezafibrate, a lipid-lowering fibrate, have been encouraging. Positive results with high-dose vitamin E (800 U/day) have been tempered by evidence that high doses may be associated with an increased risk of prostate cancer and all-cause mortality, which has limited its use. Several new medicines are currently in late-phase clinical trials and so liver-targeted pharmacological treatments are likely to be available within the next few years.
Complications
The main complication of Non-alcoholic fatty liver disease and non-alcoholic steatohepatitis is cirrhosis, which is late-stage scarring (fibrosis) in the liver. Cirrhosis occurs in the response to liver injury; such as inflammation in non-alcoholic steatohepatitis. As the liver tries to halt the inflammation, it produces an area of scarring (fibrosis) with continued inflammation, fibrosis spread to take up more and liver tissues.
If the process isn’t interrupted, cirrhosis can lead to:
- accumulation of fluid in the abdomen (ascites)
- swelling of veins of the oesophagus ( oesophageal varices), which can rupture and bleed
- confusion, drowsiness, and slurred speech (hepatic encephalopathy)
- liver cancer
- End-stage liver failure, which means the liver has stopped functioning
About 20% of people with non-alcoholic steatohepatitis will progress to cirrhosis.
Natural treatments for non-alcoholic fatty liver disease (NAFLD)
Remember, it takes years for simple fatty liver to advance to the next stages (inflammation, fibrosis, and finnaly cirrhosis). The faster you make cautions decisions, the healthier and happier your liver will feel. Here are 8 lifestyles changes that will help in natural treatments for non-alcoholic fatty liver disease:
- Focus on losing weight
- Get physical activity
- Follow a healthy and balanced diet
- Avoid the food that is not liver-friendly
- Stay clear of alcohol
- Control your blood sugar level
- Keep a check on cholesterol
- Quit smoking. Like right now.
Like any natural treatment, it takes time and patience to see the results. Following the above methods is a lifestyle change. So be strong and live healthily.
Outlook
For most people, a fatty liver does not usually cause serious worriments. To some ambit, the liver can repair itself, so switching to a healthy lifestyle will help.
Experimenters warn that NAFLD is on the increase, and if obesity continues to rise, it could become an “epidemic”.
Although simple fatty liver is not alarming, without preventive actions, some people will go on to develop NASH. And between 10 and 25 per cent of adults with NASH will go on to maturate cirrhosis within 10 years.
In the U.S. Fatty liver disease is the third cause of liver transplant, and it is on the rise.
In addition, NAFLD is linked to CVD, CKD and other conditions. Whether or not these can be inverted, even if the liver recovers, is not clear.
The best way to treat and prevent it thoroughly healthful lifestyle appraisal, with a varied and balanced diet and regular exercise.
The scientist predicts: “ Within the next 10 years, it is excepted to become the notorious cause of liver pathology, liver failure, and indications for liver transplantation in childhood and adolescence in the western world”