The Carotid Triangle
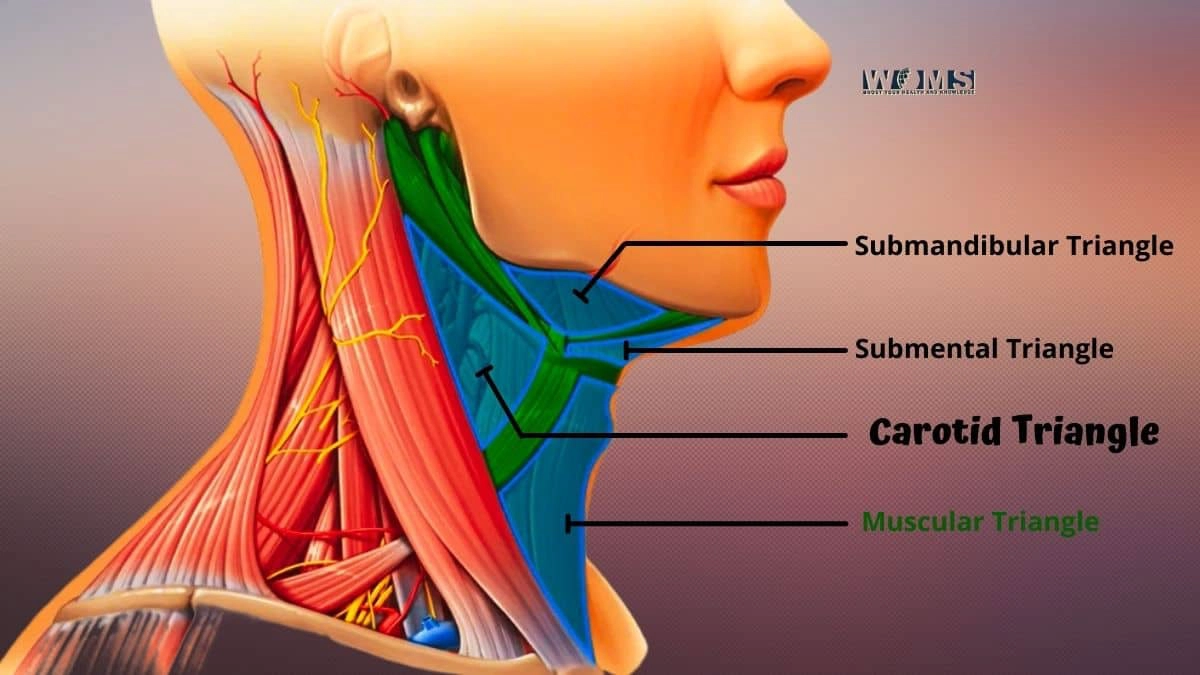
Information on the life systems of the carotid triangle is fundamental for protected and effective intercessions. So if you’re hoping to turn into an interventional radiologist or need to find out about your own body, try to become familiar with this space.
The carotid triangle is one of the matched triangles in the foremost triangle of the neck and is situated before the windpipe, among sternocleidomastoid and omohyoid muscles. It is a locale of free connective tissue simply second rate and foremost to the larynx, where the thyroid ligament starts at the cricothyroid film.
The prevalent limit is shaped by hyoid bone reaching out from midline posteriorly, with its base framing sternocleidomastoid muscle horizontally and slanted line medially; center third beginnings from the point of the mandible as set apart by lower line of the assortment of the mandible or digastric groove finishing close to mastoid interaction level; sub-par limit runs along pectoralis significant sash concealing clavicle to suprasternal indent following either side edge of sternum and ligament of the second rib.
Boundaries of the Carotid Triangle
The carotid triangle is an area of the neck that contains the carotid conduit and its branches.
The carotid triangle is limited anteriorly by the sternocleidomastoid muscle and posteriorly by the trapezius muscle. The center third of this triangle is restricted horizontally by the normal carotid conduit. Its bifurcation into outer and inside branches; is limited medially by the inward jugular vein.
- Sternocleidomastoid muscle laterally
- The common carotid artery and internal jugular vein medially
- Omohyoid muscle superiorly
Regions of the Carotid Triangle
The carotid triangle can be divided into two regions:
- The superficial zone: The superficial zone is located anterior to the sternocleidomastoid muscle,
- The deep zones: The deep zone is located posterior to the superficial zone. The carotid artery and its branches are located here.
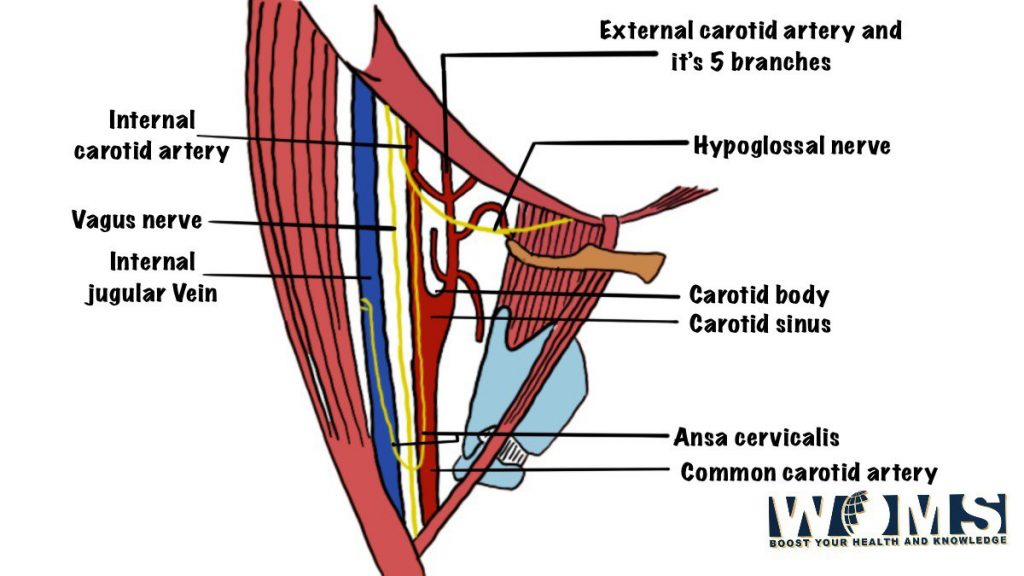
Structures Found in the Superficial Zone
The following structures are found in the superficial zone:
- External branch of the carotid artery
- The superficial branch of the facial nerve
- Auricular branch of the vagus nerve
- Occipital artery
Structures Found in the Deep Zone
The following structures are found in the deep zone:
- Common carotid artery
- Internal jugular vein
- Cervical sympathetic trunk
- Superior thyroid artery
What’s more, five designs can be found in one or the other locale
The facial nerve poorly at the level of the hyoid bone or upper third of the collection of mandible; ordinarily enters into triangle through stylomandibular tendon above omohyoid addition point on mastoid interaction in the wake of entering triangle runs anterolateral to the inside carotid conduit;
- The outside branch (back auricular) of the vagus nerve superiorly at the level of the hyoid bone in the wake of entering the stylohyoid tendon in the upper triangle enters a profound belt over sternocleidomastoid muscle and comes out on the backline about an inch underneath the ear cartilage. Structures running behind it are extra spinal nerve, prevalent laryngeal vein, phrenic vessels, ansa cervicalis.
- The occipital supply route poorly above omohyoid addition point where it enters infrahyoid muscular build with hypoglossal n.; then, at that point, runs posterolaterally toward foramen magnum;
- The normal carotid supply route and
- Interior jugular vein. The internal jugular vein is average to the normal carotid supply route. It’s critical to note that the interior jugular vein isn’t generally noticeable, as the overlying sternocleidomastoid muscle could conceal it.
Why is Carotid Triangle important?
This triangle is important because the common carotid artery ascends before bifurcating into the external and internal carotid.
Internal structures that are found in this area include:
- Internal Jugular Vein
- Common Carotid Artery (bifurcation)
- Vertebral Artery (posterior loop)
The carotid triangle also houses the carotid sinus or bulb, which contains baroreceptors that provide input to the vasomotor center in the brain.
Divisions of the Carotid Triangle
The carotid triangle can be divided into two parts:
- The superior part containing the IJV and CCA
- The inferior part contains the vagus nerve.
The carotid triangle is a locale of the neck, limited by the front and back carotid courses and their branches. It contains significant designs, for example, the normal carotid conduit, inward jugular vein, vagus nerve, and laryngeal nerves. The life structures of this area can be mind-boggling for interventional radiologists to explore to put an endovascular gadget securely ready.
The carotid triangle incorporates the normal carotid course and its bifurcation into the outside carotid conduit (ECA) and interior carotid corridor (ICA) carotid supply route, the inward jugular vein, and the vagus nerve. The normal carotid corridor is an enormous vessel that conveys blood from the heart to the head and neck. The inside jugular vein is an enormous vein that conveys blood from the head and neck to the heart. The vagus nerve controls a significant number of the muscles in the head and neck.
The carotid triangle is a significant region for interventional radiologists. We utilize this region to get to the normal carotid vein and perform methodology like angioplasty and stenting. We likewise utilize this region to get to the inside jugular vein and perform techniques, for example, thrombolysis cluster evacuation.
This region can be exceptionally hazardous if the veins are not painstakingly delineated. Without much stretch, the interior jugular vein can be harmed during carotid conduit methods, prompting intravascular coagulation and stroke.
The vagus nerve is likewise situated in this space, which controls many muscles inside the head and neck, including gulping, hacking, grinning, and so forth. Harm to this nerve has genuine ramifications for patients since it could prompt trouble with eating or talking, requiring long haul care. This should cause interventional radiologists extraordinary concern when playing out our systems on these designs nearby.
We should consistently avoid potential risks, for example, by preparing these regions before putting catheters inside them, particularly around key nerves like the vagus nerve. Assuming we cause end up hurting any design around here, we must know the seriousness of what has happened right away. This should be possible by utilizing neuro-route or asking patients how they feel later, a methodology realizing their manifestations probably won’t show for quite a long time.
The average boundary of this triangle tracks with the back midsection of the digastric muscle. At the same time, in certain patients, it is characterized by a substantial score between two muscles that are noticeable on palpation or investigation from behind. Sub-par laryngeal nerves are average to these constructions, which can be harmed during carotid conduit analysis if not distinguished as expected through imaging study before mediation.
- The carotid triangle is formed by the middle third of the sternocleidomastoid muscle anteriorly
- The apex of the triangle points posteriorly and medially at C-level (superior to cricothyroid muscle)
- The medial border follows along with the posterior belly of the digastric muscle
In some patients, it is defined by a palpable groove between two muscles that are visible on palpation or inspection from behind
Structures in the Carotid Triangle
1. The normal carotid supply route
is a huge vein that provisions oxygenated blood to the head and neck. The inner jugular vein channels blood from the mind and skull, while the vagus nerve gives engine control and tactile data to different organs in the chest and midsection. Harm to any of these constructions can be not kidding and perilous. Hence, it is significant for interventional radiologists to understand vascular life systems in the carotid triangle.
2. Inner laryngeal nerve
On the sidelong side of the vessels in the inferior laryngeal nerve (ILN), which supplies engine innervation to every one of the inborn muscles of the larynx except for the cricothyroid muscle. The ILN is in danger of injury during carotid angioplasty and stenting, given its closeness to the side of the sore.
3. The iliolumbar supply route
A part of the back division of the stomach aorta additionally enters the carotid triangle on its average boundary. This vessel emits a few branches that supply blood to the kidneys and adrenal organs. The iliolumbar supply route can be harmed during carotid mediations, so it’s essential to know its area.
4. The predominant thyroid course
In the carotid triangle, the predominant thyroid course is a significant vascular milestone. The triangle is framed by the center third of the sternocleidomastoid anteriorly, with its summit pointing posteriorly and medially at C-level (better than cricothyroid muscle).
Different supply routes found in the carotid triangle are the predominant thyroid conduit and the linguistic course. The predominant thyroid course emerges from the outer carotid conduit, while the lingual vein emerges from the interior carotid corridor. These courses can be critical when performing intercessions around here, as you want to try not to harm these constructions.
Stimulus to the carotid body
- The carotid body is stimulated by hypoxia.
- The carotid body is stimulated by hypercapnia (expanded carbon dioxide) by various blood-borne improvements, including synthetic compounds, chemicals, and synapses.
- By actual upgrades like stretch or vibration.
- It is likewise invigorated by changes in the pH of the blood.
The Carotid Body
The carotid body is a little, bean-molded construction situated on the bifurcation of the normal carotid vein into the inside and outside carotid courses. The carotid body contains chemoreceptors that are touchy to changes in oxygen (hypoxia) and carbon dioxide (hypercapnia) levels in the blood. These receptors convey messages to the cerebrum that outcome in reflex changes of breathing rate and pulse to keep up with the balance between oxygen and carbon dioxide levels in the blood.
The carotid body can likewise be invigorated by other blood-borne boosts, including synthetics, chemicals, and synapses. It is likewise invigorated by actual boosts like stretch or vibration. Changes in the pH of blood can likewise animate the carotid body.
Normal vascular anatomy in Carotid Triangle
In CT angiography
- Carotid supply routes ought to have a width more noteworthy than 0.50 cm on imaging
- Interior jugular veins ought to be under 15 mm in width
- Normal carotid supply routes ought to have an ordinary stream without any indications of stenosis (limiting)
- Trapezius muscle ought to be smooth with no calcification or mass injuries.
Moreover, any sore inside the Carotid Triangle puts patients in danger of stroke, so it is vital to know about this space when performing imaging studies.
Also Read: Anterior Triangle of the Neck
Conclusion
The carotid triangle is one of the matched triangles in the foremost triangle of the neck and is situated before the windpipe, among sternocleidomastoid and omohyoid muscles.
It is a locale of free connective tissue simply second rate and foremost to the larynx, where the thyroid ligament starts at the cricothyroid film.
This triangle is important because the common carotid artery ascends before bifurcating into the external and internal carotid
FAQs
What is the carotid triangle?
The Carotid Triangle, or predominant mediastinum, is a district in the neck where the normal carotid conduit (CCA), inner jugular vein (IJV), and vagus nerve travel through
What is the capacity of the carotid triangle?
The carotid triangle gives a physical milestone to needle situation during vascular techniques. The CCA and IJV are normally gotten to through a short, vertical cut in the lower neck just beneath the point of the jaw. The vagus nerve can be situated by touching its course parallel to the normal carotid vein.
What designs go through the carotid triangle?
The normal carotid supply route (CCA), inward jugular vein (IJV), and vagus nerve movement through the Carotid Triangle.