Understanding the Role of Nutrition in Varicose Vein Management
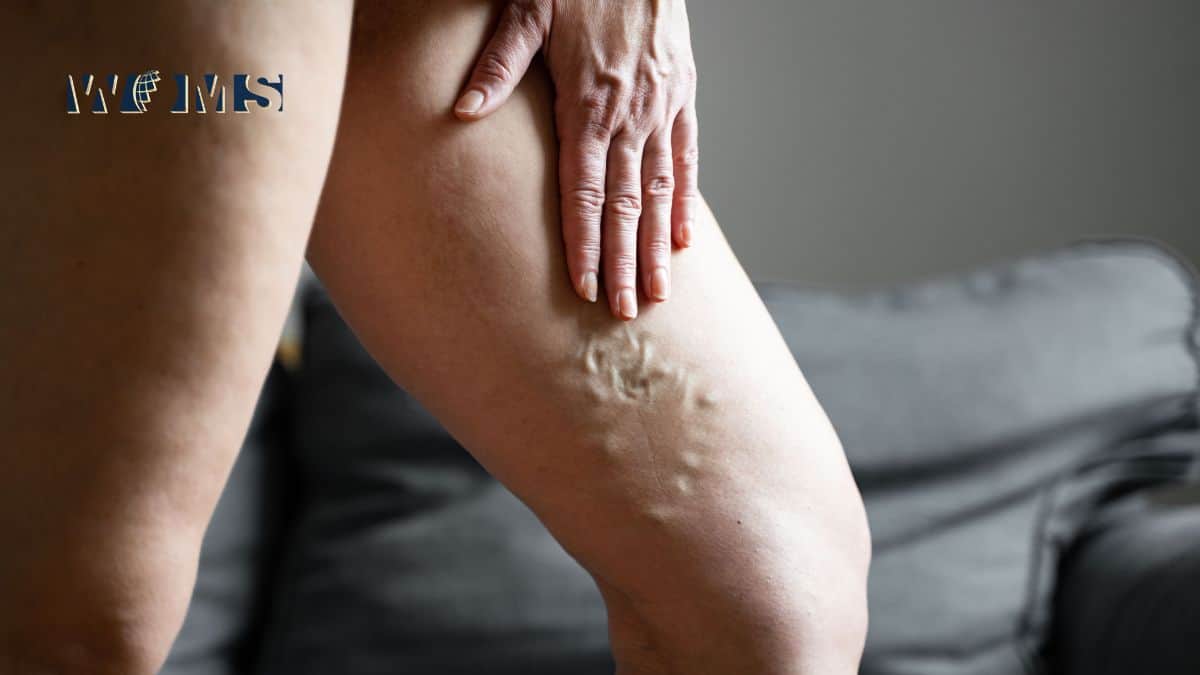
Varicose veins are a common condition that affects millions of people worldwide. They occur when the veins in the legs become swollen and enlarged. This vein deformation can cause discomfort, pain, and a range of other symptoms. While many different treatments are available for varicose veins, nutrition can also play an essential role in their management. In this article, we will explore the role of nutrition in varicose vein management. We will also provide tips on how to optimize your diet for optimal vein health.
What Are Varicose Veins?
Before we dive into the role of nutrition in varicose vein management, let’s first take a closer look at what varicose veins are.
Definition of Varicose Veins
Varicose veins are enlarged, twisted, and swollen veins that typically occur in the legs and feet. People with varicose veins may suffer from pain, swelling, and heaviness in the legs. If this condition is not treated in time, in some cases, varicose veins can lead to more serious diseases and symptoms. A vein doctor in Queens can evaluate and recommend the proper treatment for your condition.
Causes of Varicose Veins
Varicose veins can be caused by a range of factors, including:
- Age
- Genetics
- Obesity
- Pregnancy
- Prolonged standing or sitting
- Hormonal changes
- Injury
How Nutrition Affects Varicose Veins
While diet is not the major cause of varicose veins, it can influence their progression and treatment. Certain foods and dietary habits can exacerbate or alleviate varicose veins symptoms.
Nutrients That Can Help Varicose Veins
- Fiber. A high-fiber diet can help regulate bowel movements and reduce constipation, which can alleviate the pressure on veins in the legs.
- Vitamin C. This nutrient helps maintain the health of blood vessels. It can also reduce inflammation in the body.
- Vitamin E. This antioxidant may improve blood flow and reduce the risk of blood clots.
- Flavonoids. These plant-based compounds can help reduce inflammation and improve blood flow. Flavonoids are abundant in citrus fruits, berries, dark chocolate, and red wine.
Foods to Avoid
- Salt. A high salt diet can cause fluid retention, which can exacerbate swelling and inflammation in the legs.
- Processed foods. These foods are often high in salt, sugar, and unhealthy fats, which can contribute to inflammation and poor circulation.
- Caffeine. Excessive caffeine consumption can cause dehydration, which can exacerbate constipation and put additional stress on veins.
Tips for a Varicose Vein-Friendly Diet
- Consume a well-balanced diet high in fruits and vegetables, whole grains, lean proteins, and healthy fats.
- Drink plenty of water throughout the day to stay hydrated.
- Reduce your consumption of salt, sugar, and processed foods.
- Include anti-inflammatory foods and supplements in your diet.
- Avoid sitting or standing for prolonged periods. If you have a desk job, consider taking regular breaks to stretch and move around.
Other Lifestyle Changes for Varicose Vein Management
Aside from a healthy diet, there are many additional lifestyle adjustments you may make to help control varicose veins. These are some examples:
- Regular exercise. Exercise can improve circulation, strengthen veins, and help maintain a healthy weight.
- Compression stockings. These tight-fitting stockings can help improve blood flow and reduce swelling.
- Elevating your legs. When sitting or lying down, elevate your legs above heart level to improve blood flow.
- Avoid tight clothing. Tight clothing can restrict blood flow and exacerbate varicose vein symptoms.
Conclusion
Varicose veins are a common condition that can cause discomfort and pain. While there are many different treatments available, nutrition can also play an essential role in their management. By following a healthy diet rich in anti-inflammatory foods, you can help reduce varicose veins symptoms. Or you can visit New Jersey Vein Doctor for regular checkups. Besides dietary changes, you can make several other lifestyle modifications to manage varicose veins. By combining these changes with medical treatment options, you can effectively manage this condition and improve your quality of life.